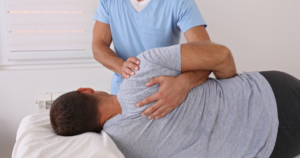
Yes, spinal decompression therapy works, but only if you have the right diagnosis and your spine is a genuine candidate for it. For patients with herniated discs and nerve compression, the results can be significant. For others, it will do very little.
Take a case we saw recently. A 44-year-old Durham project manager came to us after eight months of lower back pain radiating down his left leg. Rest, anti-inflammatories, and two rounds of physical therapy had all fallen short and his GP had started talking about surgery.
We identified a herniated disc at L4-L5 compressing the nerve root. Twelve sessions of nonsurgical spinal decompression therapy later, his leg pain had resolved and he was back to his morning runs without going near an operating table.
His outcome was not luck. It came down to the right diagnosis and the right treatment at the right time. This guide covers how spinal decompression therapy works, what the research actually says, who it helps, who it does not, the types of spinal decompression available, and what to realistically expect if you are considering it in Durham, NC.
Does Spinal Decompression Therapy Work?
For the right patient with the right diagnosis, yes. Spinal decompression therapy produces meaningful, lasting results and has a promising body of clinical evidence behind it, though studies vary in quality.
Spinal decompression is a type of traction-based therapy that gently stretches the spine to create negative intradiscal pressure inside the disc. This does two things: it encourages herniated or bulging disc material to retract toward the center of the disc, and it promotes the flow of oxygen, water, and nutrients back into the spinal discs, supporting natural healing.
For patients dealing with chronic back pain caused by disc compression, this mechanical effect can relieve pressure in a way that rest or medication alone cannot.
In our Durham practice, patients with lumbar disc herniations, sciatica, and degenerative disc disease respond most consistently to treatment. Patients with spinal stenosis caused by bony overgrowth tend to respond less predictably, because decompression addresses disc-related compression rather than structural bone changes.
The benefits extend beyond pain relief. By addressing the underlying disc mechanics rather than masking symptoms, decompression can produce structural improvement that translates to better function: reduced nerve pain in the arms and legs, improved ability to sit and sleep, and a genuine return to activity.
Many patients find relief with spinal decompression after months of failed conservative care.
The important caveat is that spinal decompression therapy is not a one-session fix. Effective protocols typically involve 12 to 20 sessions over four to six weeks.
Patients who complete the full course and follow through with rehabilitation exercises achieve significantly better long-term outcomes than those who stop early after initial pain relief.
What Does the Research Actually Say?
This is where we want to be genuinely transparent, because the research picture is more nuanced than most chiropractic websites will admit.
The honest answer is that the evidence base for spinal decompression therapy is promising but not without criticism.
Some studies have been small, some have lacked control groups, and some critics in the orthopedic community have pointed out that a portion of research has been funded by decompression equipment manufacturers, which is a legitimate concern worth acknowledging.
Here is what the more rigorous evidence shows. While no exact 2023 systematic review in the Journal of Physical Therapy Science was identified, a 2023 randomized trial found spinal decompression significantly improved pain and disability in cervical disc herniation patients compared to controls.
A study in the Journal of Back and Musculoskeletal Rehabilitation and similar research found decompression therapy outperformed or matched conventional traction for reducing leg pain caused by nerve root compression.
Studies including a 2022 paper have found that a significant proportion of patients who pursued conservative care including decompression avoided surgery at follow-up.
In terms of success, for appropriately selected patients with confirmed disc herniations or degenerative disc disease causing nerve symptoms, clinical outcomes generally show meaningful improvement in 70 to 85% of cases.
Reduced pain and improved function are the most consistently reported outcomes across studies. Success rates are lower for patients with mild to moderate spinal stenosis caused primarily by bony changes, or for those without a clear disc-related diagnosis.
Where skeptics have a point:
Back pain often becomes a catch-all term, and decompression is not an effective treatment for all types of back pain. For general non-specific lower back pain without a clear disc diagnosis, decompression is unlikely to outperform a well-structured physical therapy program.
Our position is this?
We recommend spinal decompression therapy when the clinical picture (imaging, symptom pattern, response to initial assessment) suggests disc involvement that is likely to respond. When those criteria are met, the outcomes we see in practice are consistent with what the better quality research shows. When they are not met, we say so.
What Is Spinal Decompression Therapy?
Decompression therapy is a non-surgical, non-invasive treatment that uses a computer-controlled, motorized traction table to gently stretch the spine in a targeted, precise way. It is used primarily for conditions affecting the lumbar and cervical spine.
Here is how a session works:
- You lie on a computerized decompression table, fully clothed
- A harness is fitted around your pelvis or neck depending on the area being treated
- The table applies a carefully calculated distraction force based on your body weight, the affected spinal level, and the required angle of pull
- The force cycles between peak tension and a resting phase, creating a gentle pumping action along the spinal column
- This pumping action generates the negative intradiscal pressure that draws fluid and nutrients back into the disc and helps relieve pressure on the spinal cord or nerves
Each session typically lasts 30 to 45 minutes. Most patients find it comfortable, and many find it relaxing
Nonsurgical spinal decompression is FDA-cleared in the United States. It does not involve injections, anesthesia, incisions, or recovery downtime. Patients drive themselves to and from appointments.
It is worth distinguishing this from basic traction. Traditional traction applies a constant linear pull across the spine, while spinal decompression uses variable, precisely angled force targeting a specific vertebra or spinal level, which is what creates the targeted negative pressure that basic traction cannot reliably reproduce.
How Do I Know If I Am a Good Candidate for Spinal Decompression?
This is one of the most important questions to ask before starting treatment, and a good candidate question that not every provider will answer honestly.
Patients with conditions that respond well to spinal decompression therapy generally present like this:
- Confirmed or suspected herniated disc, bulging or herniated discs, or degenerative disc disease based on MRI or clinical assessment
- Pain caused by clear nerve compression: leg pain, sciatica, arm pain, or numbness and tingle in the extremities
- Symptoms that have persisted beyond six weeks despite rest or conservative care
- No fractures, severe osteoporosis, spinal tumors, or metal hardware in the spine
- Not currently pregnant
- Able to lie flat comfortably for 30 to 45 minutes
You are likely not a good candidate if your back pain is primarily muscular, if imaging shows spinal stenosis caused by significant bony overgrowth rather than disc compression, if you have a vertebra fracture, or if you have advanced spinal instability. In those cases we will tell you, and we will direct you toward the treatment that is actually appropriate for your situation.
The most reliable path is a thorough assessment that includes your full history, a physical and neurological examination, and a review of existing imaging. A provider who recommends decompression before completing any of this is a provider worth approaching with caution.
When Spinal Decompression Does NOT Work
Most chiropractic websites will not tell you this plainly, so we will.
Spinal decompression therapy does not work well when the underlying cause of pain is not disc-related.
If your back or neck pain comes primarily from tight muscles, joint inflammation, poor movement patterns, or psychosocial factors, decompression is unlikely to produce meaningful results. It addresses disc and nerve compression specifically, not back pain as a general category.
It also does not work well as a standalone intervention. Patients who complete decompression sessions without rehabilitation exercises, postural correction, or lifestyle modification tend to experience shorter-lived results.
The decompression creates a window of opportunity for the disc to heal and the spine to stabilize your overall health improvements; what you do in that window determines how long those improvements last.
Around 15 to 30% of appropriately selected patients do not achieve the response we are looking for. That is not a failure of the treatment so much as a reminder that no conservative therapy has a 100% success rate.
On the question of whether it can make things worse: for the vast majority of appropriately screened patients, no. The most common negative response is temporary muscle soreness in the first two to three sessions as the muscles supporting the spine adjust.
A more concerning response (increased nerve pain, worsening symptoms, or new neurological changes) is rare and almost always signals either a missed contraindication or a more serious underlying condition. This is why proper screening is non-negotiable.
Conditions where decompression carries genuine risk include:
– Severe osteoporosis
– Spinal instability
– Active spinal infections
– Certain presentations of spinal stenosis
These are absolute contraindications. Any reputable provider screens for all of them before starting treatment.
How Long Does It Take for Spinal Decompression to Work?
This is the question patients actually want answered, and the honest answer is that it varies, but there are useful benchmarks.
Most patients notice some reduction in symptoms between sessions three and six. This is often reported as reduced nerve pain in the legs or arms before the back pain itself improves, which reflects nerve root decompression beginning to take effect. If you reach session six with no change at all, that is a signal worth discussing with your provider.
Meaningful functional improvement (being able to sit longer, sleep better, return to light activity) typically occurs between weeks two and four for patients who are responding well.
Full resolution of symptoms, where it occurs, usually happens toward the end of the full protocol or in the weeks following completion as the disc continues to heal and the spine continues to adapt.
A 28-year-old warehouse worker from Durham came to us barely able to sit for more than ten minutes due to a herniated disc at L5-S1. By session five he was sleeping through the night. By session fourteen he had returned to full duties at work.
His case is not unusual for a well-selected patient who commits to the full protocol and manages contributing factors consistently between visits.
Surgical and Nonsurgical Spinal Decompression: Types of Spinal Decompression and How They Compare
Understanding the surgical and nonsurgical options is important before committing to any treatment path.
The types of spinal decompression available range from fully conservative to major surgery, and where you land on that spectrum should be determined by the severity of your condition and how your spine has responded to previous care.
Nonsurgical spinal decompression (the computerized traction-based therapy discussed throughout this article) is the appropriate starting point for most patients with disc herniations, degenerative disc disease, and nerve compression without progressive neurological deficits. It is non-invasive, carries minimal risk, and has a meaningful evidence base for the right candidates.
Surgical spinal decompression becomes a consideration when conservative care has been exhausted, when neurological deficits are progressing, or when structural changes to the spine require direct intervention. The main types of treatment in the surgical category include:
- Laminotomy or laminectomy: Removal of part (laminotomy) or all (laminectomy) of the lamina to relieve pressure on the spinal canal and spinal nerves. Laminectomy is more extensive and commonly used for spinal stenosis.
- Foraminotomy or foraminectomy: Enlargement of the foramen (the opening where nerve roots exit the spine) to relieve nerve root compression caused by bone spurs or a narrowed foramen.
- Spinal fusion: Stabilization of two or more vertebrae to eliminate movement at a painful or unstable segment, often performed alongside decompression surgery.
- Minimally invasive surgery: Surgical options using smaller incisions and specialized instruments to decompress the spine with less tissue disruption and faster recovery.
Surgical options carry real risks including infection, anesthesia complications, scar tissue formation, and the possibility of adjacent segment degeneration following spinal fusion. They are appropriate when they are appropriate, and not before.
For patients with mild to moderate spinal stenosis, a herniated disc, or degenerative disc disease, a genuine course of nonsurgical spinal decompression should be the first treatment option explored. In our Durham clinic, we have seen patients avoid surgical options they were told were inevitable by committing fully to a structured conservative treatment plan.
What Are the Risks of Spinal Decompression?
Non-surgical spinal decompression therapy is considered low-risk when performed by a qualified provider on an appropriately screened patient. Serious adverse events are uncommon, and its safety and effectiveness profile compares favorably to surgical alternatives.
The most frequently reported side effect is mild muscle soreness in the first week of treatment, similar to post-exercise soreness. This is not a warning sign in most cases and typically resolves as the body adapts to treatment.
More significant risks are almost always associated with contraindications that should have been identified at screening. Performing decompression on a patient with a vertebra fracture, severe osteoporosis, spinal instability, or active infection is the source of most documented adverse outcomes, not the therapy itself when properly applied.
Risks worth discussing with your provider before starting include temporary symptom flare in the first few sessions, and the small possibility that decompression reveals a more serious underlying issue that requires a different treatment pathway. In those cases, identifying the issue is a better outcome than continuing to treat the wrong problem.
What Happens If Spinal Decompression Doesn’t Work for Me?
This is a question we appreciate patients asking because it tells us they are thinking clearly rather than just hoping for the best.
If you complete a full, appropriately structured course of spinal decompression therapy and do not achieve the response we are looking for, there are clear next steps and it is not a dead end.
The first step is reassessment. If pain doesn’t resolve as expected, we want to understand why. Has the diagnosis changed? Is there a component we underestimated (facet involvement, central sensitisation, a psychosocial factor contributing to chronic pain persistence)? Updated imaging including MRI may be warranted.
Depending on what reassessment shows, next steps might include a referral for pain management consultation, a course of targeted physical rehabilitation, a referral for a surgical opinion, or a combination approach that addresses factors we were not fully treating initially. The goal at every stage is to ease your pain and get you back to the life you want to be living.
What we do not do is keep running the same protocol and hoping for a different result. If decompression is not working, the honest and responsible thing is to say so, investigate why, and adjust accordingly.
Frequently Asked Questions
For appropriately selected patients with confirmed disc herniations or degenerative disc disease causing nerve symptoms, clinical outcomes generally show meaningful improvement in 70 to 85% of cases.
Pain levels reduce and function improves in the majority of well-selected patients. Success rates are lower for patients with spinal stenosis caused primarily by bony changes or for those without a clear disc-related diagnosis. This is why candidacy assessment matters more than any headline success figure.
More is not better with spinal decompression. The treatment works through a cycle of tension and rest that allows disc tissue to rehydrate and heal between sessions. Daily sessions do not allow adequate recovery time and can lead to tissue irritation and increased soreness rather than accelerated healing.
Standard protocols space sessions across the week for this reason, typically three to five times in the initial phase and tapering as improvement occurs. Following your provider’s recommended schedule is one of the most important factors in achieving reduced pain and lasting results.
In the hours following a session, avoid prolonged sitting, heavy lifting, and high-impact activity. The disc tissue is in active recovery immediately after treatment, and loading the spine aggressively during this window can reduce the benefit of the session.
Light walking is fine and often encouraged. Consistent attention to posture, sleeping position, and core engagement between sessions significantly influences overall outcomes and helps relieve symptoms over the full course of treatment.

Meet Dr. Kevin McLaughlin
Dr. Kevin McLaughlin is the owner of Complete Chiropractic Sports and Wellness and has been serving the Triangle community since 2012. Originally from Shenandoah Junction, West Virginia, he graduated from Palmer College of Chiropractic and opened his practice with a focus on natural, holistic healing.
He takes a comprehensive approach to care, specializing in techniques such as Cranial Facial Release, spinal decompression, dry needling, shockwave therapy, and cold laser therapy. His philosophy centers on treating the body as a whole and addressing the root cause of pain, rather than just managing symptoms.
Dr. McLaughlin is passionate about helping patients move better, feel better, and live healthier lives, while supporting each individual’s long-term wellness goals.
Outside the clinic, he enjoys golf, staying active, music, and the outdoors, and is a proud father to his two children, River and Aria.